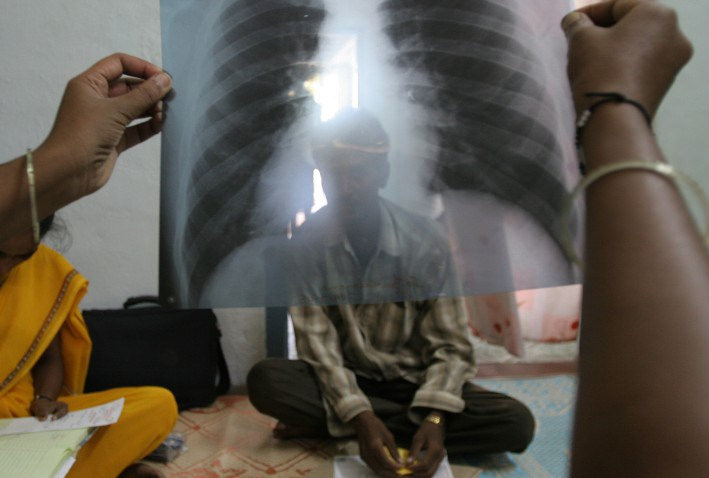
Link found between gum disease and rheumatoid arthritis
03/21/2019 / By Lance D Johnson
We tend to forget the commensal relationship we share we bacteria. Our bodies are home to colonies of bacteria which benefit us in various ways, including interacting, coordinating, and coordinating vital functions. As beneficial as this relationship is, it can also be delicate: Hypochondriac mindsets have led to over-sterilization and overuse of synthetic antibiotics that indiscriminately destroy these commensal bacteria biomes.
The endangerment of valuable bacteria species ultimately allows infectious pathogens to colonize and dominate our immune systems. Studies are quickly shifting to discover and learn more about these beneficial bacteria life forms, the vital roles they play, and how disease manifests in their absence.
Infectious bacteria found in gum disease also play a role in rheumatoid arthritis
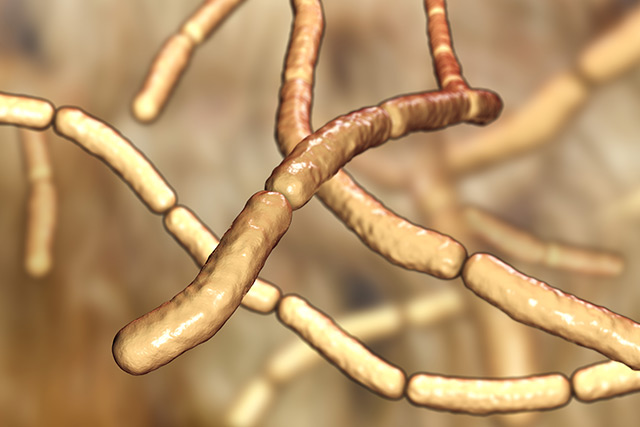
Researchers from Johns Hopkins University have found a type of infectious bacteria that is taking over depleted microbiomes, which could trigger both severe gum disease and rheumatoid arthritis. They report that the bacteria Aggregatibacter actinomycetemcomitans are found in roughly 33 percent of people and are predominant in patients with periodontal disease and/or rheumatoid arthritis.
The team found evidence that 47 percent of patients experiencing rheumatoid arthritis also were infected with the same bacterium that is causing their periodontal disease. At first, the researchers recognized a pattern of damage taking place in the gums of patients with periodontal disease similar to what’s seen in the joints of rheumatoid arthritis patients. In periodontal disease, the bacteria spurs the production of citrullinated proteins, which initiate an antibody response.
The emergence of this bacterium elsewhere, in the joints, causes an inflammatory response with the body’s immune system. The bacterium causes cells called neutrophils to inflame the immune system, rendering a vicious auto-immune response. This causes conditions we recognize as rheumatoid arthritis, which can be felt as pain in the joints, or even inflammation around the heart and lungs. Dr. Felipe Andrade, a rheumatologist at Johns Hopkins who oversaw the research, said that while he and his team couldn’t figure out how the bacteria travel from the mouth to the joints, the connection was there.
A paradigm shift is needed in our relationship with bacteria and our own immune system
The National Institute of Arthritis and Musculoskeletal and Skin Diseases says an estimated 1.5 million Americans now live with rheumatoid arthritis. As with any disease-causing bacteria, conventional advice given by doctors to their patients is sterilization, chemical hygiene, and antibiotics. While possibly effective in the short term, this approach only causes a vicious cycle for other infectious bacteria to colonize in the future. The secret to maintaining good health long term is in knowing how to respond to infections without damaging the commensal relationship that we share with all bacteria, both good and bad. The further we separate from these natural relationships, the closer we get to manifesting disease in the body.
The current medical treatments for rheumatoid arthritis only suppress the immune system of the patient, welcoming future infections. In much the same way that we discourage commensal bacteria from establishing on us and in us, medical treatments discourage the patient’s own immune system from strengthening, which also beckons future infections. For patients to truly heal, the vicious cycle of disease management, weakening of the immune system and destruction of the bacteria microbiomes must end. This would require a drastic paradigm shift in thought and how we respond to pathogens in our prevention strategies. (Related: The mouth is a first responder for the immune system: New study provides clues for how the body defends against oral invaders.)
Sources include:
Tagged Under: commensal bacteria, infection, microbiome, periodontal disease, rheumatoid arthritis